UNITED NATIONS, New York – Two thousand years ago, doctors hypothesized that women’s reproductive organs were the same as men’s, only inside-out. Four hundred years ago, doctors speculated that the uterus might wander out of place, causing women’s emotions to go awry. Today, science has largely solved the mysteries of the female body… right? Wrong.
Modern medical science continues to regard women’s bodies and health, and especially their reproductive system, as enigmatic: Research on the medical index PubMed is four times more likely to describe women, and their bodies, as “mysterious” compared to men.
What are the consequences of knowing less about the bodies of women than men? Women suffer longer before their ailments are diagnosed – even when their illness and symptoms are the same as men’s. Women are more likely to experience chronic pain, but are less likely to have their pain believed and treated in clinical settings. Overall, women spend 25 per cent more of their lives in ill health compared to men.
Next week, world leaders will convene at United Nations Headquarters in New York to explore the promise of technology, research and innovation in advancing global development. There, UNFPA, the United Nations Population Fund – the sexual and reproductive health agency of the UN – will urge those leaders to use the transformative power of science, technology and innovation to answer long neglected questions about women’s and girls’ health.
Below are five ways the world can, and must, close the gender health gap.
1- Prioritize women’s health in medical research.
For too long, most medical research has been conducted using white men as the standard. Women have been historically excluded from clinical trials for disease treatment, for example.
One commonly cited reason is researchers’ fear that these trials could pose risks to a woman’s pregnancy, a valid concern. But it raises questions around whether women are being fully regarded as decision-making agents over their own bodies: One evaluation found that research institutions and scientists have a “distrust of women to prevent pregnancy” while participating in a clinical trial. Some impose high burdens of proof, like confinement periods, as a condition for women’s participation.
And of course pregnant women also experience illness and require treatment, but only 4 per cent of clinical trials in the past decade have included pregnant women. They need to be protected through research, not from research, experts say.
The result is that our understanding of women’s bodies has lagged behind. Many medication dosing guidelines are based on the bodies of men, for example, leading to more adverse drug reactions in women.
These gaps in knowledge also lead to further gender bias when women seek care. Doctors are more likely to dismiss their complaints, something known as medical gaslighting. Women are more likely to be considered “emotional” or suspected of lying about their symptoms. They are also more likely to have their conditions described as “medically unexplained”.
These biases are often worse for women experiencing other forms of marginalization, such as racial and ethnic discrimination, disability, or poverty.
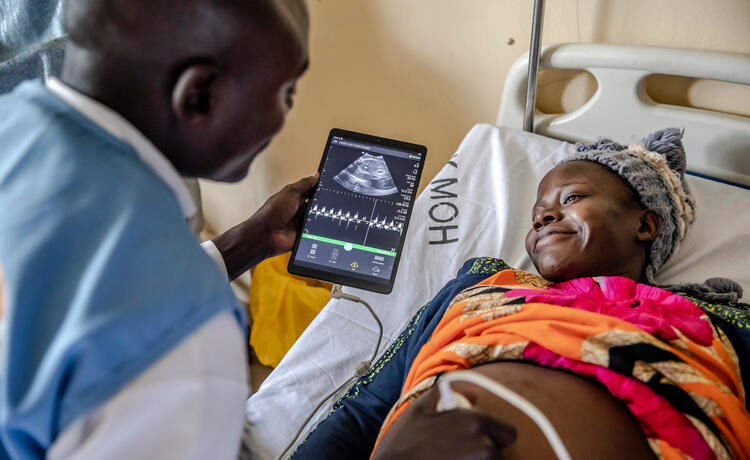
2- Close the diagnosis gap.
Women are more likely than men to experience misdiagnosis and delayed diagnosis for conditions ranging from heart problems to attention deficit/hyperactivity disorder. And delayed detection and treatment are especially common when it comes to health conditions exclusive to women.
Women with endometriosis spend an average of 10 years suffering from this debilitating condition before being diagnosed, even when they have “clear symptoms”, doctors say. Up to 70 per cent of women with polycystic ovarian syndrome are also undiagnosed, even though this condition can cause extreme pain and infertility. Globally, it is estimated that for every woman diagnosed with a female-specific health condition, an estimated four remain undiagnosed.
Underdiagnosis can be worse for women and girls with poor access to quality health care, such as those in crisis settings. Halima, a girl in Maiduguri, Nigeria, told UNFPA about enduring menstrual pain so intense she is sometimes unable to stand. Such pain can be a sign of a serious underlying condition, but diagnosis and treatment were out of reach for Halima, whose family had to flee conflict and restart their lives in a new location.
The emotional and financial stress made things even worse: “It is even more difficult each time of the month to cope with the severe menstrual pain, do housework, attend school and concentrate in class,” she said.
Lack of diagnosis, delayed diagnosis and misdiagnosis worsen health outcomes. This is not only a form of health inequity – it can also be a death sentence.
The World Health Organization finds that roughly a quarter of all maternal deaths are linked to undetected conditions, such as infections or chronic diseases, that would have been manageable if diagnosed in time.

3- Understand the costs – which are ultimately borne by all of us.
When we recognize the staggering cost of inaction, the need to act becomes undeniable. A recent report by the World Economic Forum highlights the many ways in which the women’s health gap harms individuals, communities and the global economy.
Poor health and disability lead to women and girls losing access to education and economic opportunities – losses that are passed down to the next generation in the form of worse financial security and health. By contrast, addressing women’s ill health could boost women’s workforce participation, economic empowerment and the overall welfare of their families.
The report estimates that reducing women’s poor health by approximately two thirds would yield at least $1 trillion to the global economy annually by 2040, and this is believed to be a conservative estimate.
That means that perpetuating the women’s health gap could, conservatively, cost the world some $1 trillion per year – to say nothing of the lost labour, ingenuity, creativity and innovation that the world might see when billions of women are freed from unnecessary pain, illness and death.

4- Address the gender data gap.
In many ways, the gender health gap starts with a failure to ask the right questions. Do illnesses present differently in women versus men? Are we consistently measuring symptoms of menopause, menstruation and pain?
The World Economic Forum report finds that the gender data gap starts at the very beginning of data collection and spans all the way to the clinic – and even the grave. During one month of the global COVID-19 pandemic, researchers noted that only 37 per cent of countries had reported sex-disaggregated mortality data.
Failure to measure women’s health burdens means they are systematically underestimated – which affects how much investment companies and governments are willing to spend on solutions.
And data analysis itself can dilute the visibility of women in large datasets, with AI-powered assessments shown to perpetuate bias when programmes are not carefully designed and monitored to ensure equity.
5- Inclusion is the solution – and it benefits everyone.
The solution to the gender health gap, as to so many things, is inclusion: More inclusion of women in studies, more inclusion of women in the research field, more inclusion of women in positions of leadership.
Fortunately, there is progress underway, a recent impact report shows: Health investors are increasingly requiring sex, gender and pregnancy-inclusive research and development. Many are pledging funds for women-centric research and innovation.
UNFPA’s Centre of Excellence for Civil Registration and Vital Statistics Systems is working with governments and partners at the level of data collection. This programme aims to help countries be more gender-responsive in the registration of birth, marriage, divorce and death statistics. Improved and inclusive data can help to measure disparities in legal identity systems, health outcomes and other inequalities.
And experts are increasingly calling for equitable design and evaluation of AI and other technologies, which can improve everything from data analysis to diagnostic tools and treatments.
The tools are available, the path forward is clear.
“It is time to close the persistent gaps in health, equity and economics that prevent medical innovations from reaching the most vulnerable,” said Ms. Diene Keita, Executive Director of UNFPA. “A healthier future for all starts with investing in women’s and girls’ health today.”


